Prevalence of diarrhea caused by Cryptosporidium parvum in non-HIV patients in Jeollanam-do, Korea
Article information
Abstract
The present study investigated the prevalence rate of Cryptosporidium parvum as a cause of diarrhea. We examined 942 stools of unidentified reasons occurring in patients in whom no immunosuppression had been detected. We examined the stools for Cryptosporidium parvum via modified acid-fast staining. The clinical records of all of the positive patients were then analyzed. Nine (1%) of the stools among the 942 diarrheal patients were positive for C. parvum. The positive rate in the males was 1.1% (6/522) and the positive rate of the females was 0.7% (3/420). Age distribution revealed that the highest positive rates were in patients in their sixties, with a positive rate of 2.5% (4/158). In the clinical tests, levels of c-reactive protein, erythrocyte sedimentation rates, and neutrophil proportions were normally increased in the peripheral blood, whereas the lymphocyte proportion exhibited a tendency towards decrease. The pathological findings were compatible with an inflammatory reaction in the host.
Cryptosporidium parvum is a common protozoan pathogen with worldwide distribution, and causes severe and life-threatening diarrhea in immunocompromised hosts. Although this protozoan is far more common in immunocompromised patients, it is also known to induce diarrhea in immunocompetent persons, albeit for a short period. Cattle are known to be a source of Cryptosporidium infections, but environmental waters are also an important source of Cryptosporidium (Smith and Rose, 1998). In fact, the huge outbreak of South Milwaukee, in 1993, has been determined to be the result of waterborne cryptosporidiosis (Mackenzie et al., 1994). In a previous study, 6.1% of diarrheal patients in developing countries and 2.1% of diarrheal patients in developed countries were determined to have been infected with Cryptosporidium, whereas the infection rates among HIV-positive diarrheal patients were significantly elevated, at 24% in developing countries and 14% in developed countries (Adal et al., 1995). In Korea, there is currently no data available regarding the prevalence of diarrhea due to C. parvum infections in immunocompetent persons. In this study, we have investigated the prevalence of C. parvum as a cause of diarrhea in individuals without a particular history of immunosuppression, and then analyzed the clinical data of those persons.
Fecal samples of diarrheal patients in whom the etiological diarrheal agent has not been identified were transferred to the Jeollanam-do Institute of Health and Environment from local hospitals, between August 2003 and July 2004, in an effort to identify the causative agents. A total of 942 fecal samples were included in this study, 522 of the samples came from males, and 420 came from females. All of the patients from whom samples were collected resided inside Jeollanam-do, in locations including Naju-si, Mokpo-si, Suncheon-si, Hwasun-gun, and Haenam-gun.
Fecal smears were prepared from each sample via formalin-ether concentration, stained by a modified acid-fast staining, and examined for the presence of C. parvum oocysts. Oocysts of 4-5 um in diameter, red in color and containing sporozoites were considered to be C. parvum oocysts. Statistical analyses were conducted via Student's T-tests. The medical records of all of the patients considered to be positive for C. parvum were also analyzed.
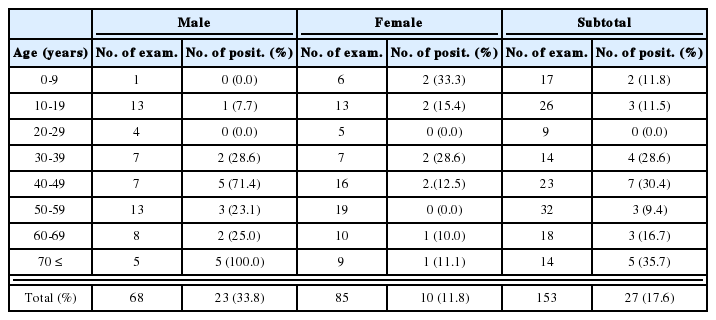
The stool samples of patients with diarrhea of unidentified etiology were transferred to the Jeollanam-do Institute of Health and Environment from local clinics, for further evaluation. The overall positive cryptosporidiosis rate among the 942 diarrheal patients was determined to be 1%. The positive rate in the males was 1.1% (6/522) and the positive rate in the females was 0.7% (3/420). The sex of the patients was not found to be a statistically significant factor (P > 0.5). Age distribution, however, revealed that the highest positive rate was in patients in their sixties, at 2.5% (4/158). Among the nine patients who tested positive for Cryptosporidium, only one was under 10 years old, and all of the rest were over 30 years of age. The highest positive age group in males was patients in their sixties, at 4.1% (3/74), and the highest positive age group among females was patients in their seventies, at 3.8% (2/53) (Table 1).

Age distribution of cryptosporidiosis among immunocompetent diarrheal patients examined by modified acid-fast staining, between August 2003 and July 2004
We also attempted to characterize seasonal variations in the incidence rate of Cryptosporidium diarrhea. Cryptosporidium diarrhea was found to occur primarily between March and April (2.1-2.8%) and between July and September (2.9-4.3%). The peak incidence rate was in September (4.3%). Diarrhea also occurred in January also, albeit at a lower incidence rate (1.3%) than in spring or summer.
We reviewed the medical records of the nine Cryptosporidium-positive patients, in order to detect a possible specific clinical correlation with C. parvum infection. One of the nine positive patients suffered from pulmonary tuberculosis (TB), and two of the patients were hypertension (Table 2). The others had acute duodenal ulcers or gall stones. Only one of the nine patients had a history of food poisoning, after visiting a neighbor's house one week before the onset of diarrhea (patient 2). The majority of the patients complained of nausea, vomiting, and abdominal pain, in addition to their diarrheal symptoms, and received negative results on stool occult blood and parasite ova tests. The duration of the diarrhea in these patients was 6 to 18 days, with some individual differences. During this period, in three out of five patients the proportion of lymphocytes in the complete blood count (CBC) test was found to be reduced, with levels 3.8-15.8% lower than normal range (20-40%). The majority of the patients were admitted to the hospital for one week, and their diarrheal symptoms had normally been resolved by the time of discharge. Conversely, the proportion of neutrophils was elevated in three of five patients, to 76.3-83.4% above normal range (30-70%). The proportion of lymphocytes was not uniformly reduced, however, as an increased lymphocyte proportion was detected in two of the patients. We also assessed the erythrocyte sedimentation rate (ESR) and the c-reactive protein (CRP) levels, as inflammation indicators. The ESR values were normally elevated (100-109 mm/hr) above normal (0-15 mm/hr) in these patients. The CRP levels were also generally elevated (3.3-18.2 mg/dL), but not in all cases. A jejunal biopsy conducted on one patient resulted in a pathological finding of inflammatory intestinal mucosa with erosion. Abdominal ultrasonography performed on another patient revealed mild to moderate diffuse wall thickening in the small and large bowel loops.
In a previous study, we determined that 8.2% of inhabitants in Jeollanam-do were infected with C. parvum (Yu et al., 2004). Another epidemiological study, conducted in the same region, revealed that 10.6% of residents were infected with C. parvum (Chai et al., 1996). However, the majority of these previous epidemiological studies suffered from a paucity of clinical information regarding the patients who tested positive for C. parvum. In this study, we collected only diarrheal stools, and attempted to obtain sufficient clinical data for the C. parvum positive patients, in whom we had confirmed these infections via stool examinations. In this study, only 1.0% of the studied diarrheal patients was positive for C. parvum infections. It was previously determined that 6.1% of diarrheal patients in developing regions, and 2.1% of diarrheal patients in developed regions, had been infected with Cryptosporidium (Adal et al., 1995). On the basis of the findings of the present study, it can be concluded that Cryptosporidium diarrhea occurs less frequently in Korea than in other developed countries. Recently, 10.5% of HIV-infected patients were reported to be positive for C. parvum infection (Guk et al., 2005). From this result, it seems to be that diarrhea in immunocompromised patients with Cryptosporidium infections occurred at a rate ten times as high as that seen in immunocompetent patients in Korea.
With regard to the clinical data, elevated ESR or CRP scores were considered to reflect some type of inflammation existing inside the body (Lab Tests Online). Increased neutrophil proportions might indicate a response to C. parvum infection (MedlinePlus). However, it remains unclear as to whether or not decreased lymphocyte proportions are the cause of the infection, or constitute part of a response to the infection. Increases in neutrophils and decreases in the lymphocytes were maintained in the patients from the beginning of the diarrheal period, until the diarrhea had subsided. Interestingly, all nine of the C. parvum-positive patients discerned by our tests had previously received negative results for stool parasite ova or protozoa at the local clinics at which they had initially been examined. Therefore, it can be concluded that the results of stool examinations for the detection of parasite ova at the local clinics in this area are fairly unreliable.
The records on pathological findings of one of the positive patients showed nonspecific colitis with diffuse mucosal hyperemia and scattered whitish exudates, and inflammatory mucosa with erosion in the small intestine with no mention of Cryptosporidium. These pathological findings were consistent with the findings of CBC, which indicated nonspecific inflammation.
In conclusion, 1% of diarrhea occurring in immunocompetent patients in Korea was determined to be caused by C. parvum infection. These patients exhibited nonspecific inflammatory findings on CBC tests and on pathological examinations conducted via endoscopy or abdominal ultrasonography. The diarrheal symptoms in these patients persisted for a period of between 6 and 18 days, and were alleviated solely by symptomatic treatment. All of the patients infected with C. parvum had not been diagnosed at the initial primary care clinics.
References
Notes
This study was supported by a grant from the Korean Science and Engineering Foundation [R04-2001-000-00203-0(2003)].